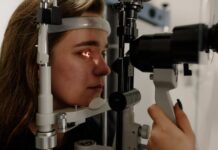
Investing in a vision screening device is a significant decision for clinics, schools, occupational health providers, and community outreach programs. Because early detection is the cornerstone of preventing long-term vision impairment, the quality of your equipment directly impacts your ability to provide effective care.
However, the market is saturated with various technologies, ranging from simple manual tools to advanced automated systems. Selecting the wrong device can lead to wasted capital or, more critically, inaccurate results that miss underlying health issues. To ensure you make an informed investment, follow these seven strategic steps.
1. Define Your Specific Use Case
Before looking at hardware, you must define your operational requirements. A “one-size-fits-all” approach rarely works in clinical diagnostics. Ask yourself:
– Who is the target demographic? (e.g., children requiring pediatric-specific interfaces, or elderly patients needing different acuity scales).
– What is the environment? (e.g., a controlled clinical setting vs. a mobile outreach unit).
– What is the expected volume? (How many screenings must be completed per day?).
Defining these parameters prevents the two most common procurement errors: overspending on high-end features you won’t use, or purchasing a device that lacks the throughput necessary for your workload.
2. Vet the Provider, Not Just the Product
A vision screener is more than a piece of hardware; it is a long-term partnership. When evaluating companies like Depisteo or other industry players, look beyond the spec sheet.
– Longevity: How long has the company been in the industry?
– Support Ecosystem: Do they offer technical support, software updates, and training?
– Reliability: A provider with a proven track record is essential for minimizing downtime.
3. Conduct Thorough Digital Research
Once you have a shortlist of potential providers, use their official websites to perform a deep dive. Official product documentation often contains technical details—such as specific testing protocols and hardware specifications—that marketing brochures might gloss over. Use this phase to eliminate any providers whose technology does not align with the needs you identified in step one.
4. Verify Reputation and Clinical Trust
In healthcare, reputation is a proxy for reliability. Do not rely solely on a company’s self-reported claims.
– Client Reviews: Seek out feedback from actual users in your specific field (e.g., school nurses or occupational therapists).
– Clinical Validation: Ensure the device is recognized and validated by professional standards. A device’s reputation is built on its ability to produce consistent, repeatable, and accurate results.
5. Prioritize Key Technical Features
When comparing models, focus on the features that drive clinical outcomes and operational efficiency:
– Accuracy and Validation: This is non-negotiable. The device must be clinically validated to ensure it detects vision problems reliably.
– Portability: If you are conducting outreach or school visits, a lightweight, rugged design is essential.
– Scalability: The device should be able to handle your projected daily volume without lagging or requiring excessive recalibration.
6. Evaluate User Experience (UX) and Automation
A device is only as effective as the person operating it. To minimize human error and maximize efficiency, prioritize simplicity over complexity.
– Automated Measurements: Look for devices that reduce manual input, which minimizes the risk of data entry errors.
– Intuitive Interface: The software should be easy to navigate, providing clear, actionable results that can be quickly interpreted by staff.
– Minimal Training: A device that is easy to use reduces the time and cost required to train new personnel.
7. Perform a Value-Based Cost Analysis
While budget is always a factor, the cheapest option is rarely the best investment. When comparing costs, look at the total value of ownership. This includes:
– The initial purchase price.
– Costs for consumables or maintenance.
– The cost of software updates.
Note: Always prioritize clinical accuracy and device quality over the lowest price point. An inexpensive device that yields inaccurate results is a liability, not an asset.
Conclusion
Selecting a vision screener requires balancing clinical accuracy with operational reality. By defining your specific needs, vetting providers thoroughly, and prioritizing ease of use, you can invest in technology that improves patient outcomes and streamlines your workflow.